Community Health Needs Assessment (CHNA) and Community Health Implementation Plan (CHIP) Reports
Everyone should get the chance to live their healthiest lives. At Rush University System for Health, we know that good health is shaped by more than medical care. It’s also about access to building blocks of health like safe and affordable housing, quality education, nutritious food and family-supporting jobs. That’s why we’re committed to working alongside community members, local nonprofit organizations and public partners to address the root causes of health inequities.
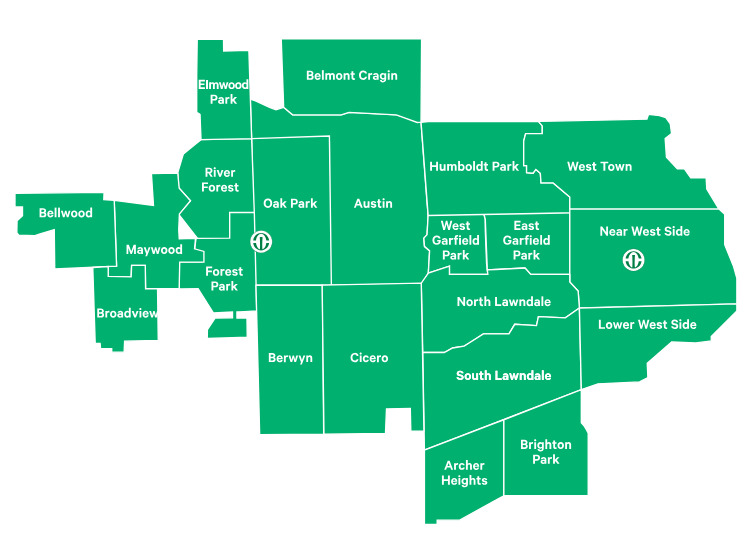
Rush’s 2025 CHNA and 2026–2028 CHIP reflect what we’ve learned by listening to the voices of the 21 communities we serve and combining that input with the information highlighted in our interactive community profiles.
Our work to advance health equity is grounded in trust, shaped by data and guided by the lived experiences of residents. Together, we’ve identified shared priorities and created strategies that respond to what community members say they need most.
Nurturing healthier neighborhoods takes time, care and collaboration. We invite you to explore the Rush CHNA and CHIP, which outline our goals, the steps we’re taking and the progress we’re measuring along the way. They document how we’re working together to create a future where everyone has the opportunity to thrive.
Community Benefit Highlights
At Rush University Medical Center and Rush Oak Park Hospital, our commitment to improving health outcomes goes far beyond clinical care. As part of the Rush University System for Health, we are proud to present the 2024 Community Benefit Highlights—a reflection of our ongoing efforts to advance health equity and strengthen the well-being of the communities we serve.
These highlights showcase the impact of our Community Health Needs Assessment (CHNA) and Community Health Implementation Plan (CHIP), as well as the strategic investments made through our Anchor Mission. From addressing social determinants of health to fostering partnerships that support neighborhood vitality, this report captures the meaningful ways Rush is working to ensure that everyone has a fair and just opportunity to live a healthy life.
- Community Benefit Report FY2024
- Community Benefit Report FY2023
- Community Benefit Report FY2022
- Community Benefit Report FY2021
- Community Benefit Report FY2020
- Community Benefit Report FY2019
- Community Benefit Report FY2018
- Rush’s Community Benefits Summary for 2017 is a report on work guided by the 2017-2019 CHIP. Rush invested $335 million in community benefits in 2017 across a range of efforts, including research, donations, Medicare/Medicaid programs, Charity Care and more.
- Community Benefit Report FY2017
- Anchor Mission Playbook explains Rush's role as an anchor institution and shares the approach behind Rush's Anchor Mission Strategy
- What We Heard: Coming Together to Improve Health and Wellness on the West Side is a report that arose from a January 2017 meeting and 21 community conversations about health disparities and other inequities with stakeholders who work, live and congregate on the West Side. The foundational document of West Side United, this report summarizes the opportunities for improving health on the West Side and the feedback community members provided about the collaborative’s proposed goals.
- 2018 Health Equity Report: Patient Care Through An Equity Lens* examines who visits Rush for care, the conditions that bring people through our doors and how their outcomes reflect public health trends around health disparities that are largely related to race and ethnicity. This report, the first of its kind for Rush, is a launchpad for our work to continue improving the equitable delivery of health care to the communities we serve.
*Resources in the following list were used to inform the 2018 Health Equity Report: Patient Care Through An Equity Lens:
- Rush patient maps
- Technical notes (includes definitions, methods information, project operationalization details)
To learn more about health equity nationwide and in Chicago, visit the following:
- Healthy Chicago 2.0: Partnering to Improve Health Equity 2016 - 2020
- Institute for Healthcare Improvement videos:
- Metropolitan Planning Council report: The Cost of Segregation
- Robert Wood Johnson Foundation report: What Is Health Equity?
Contact Us
For more information about our CHNA, CHIP or CBR, please contact:
Julia Bassett
System Manager, Community Health and Benefits
julia_s_bassett@rush.edu

